In case you missed the update about this pregnancy being considered high risk, you can read it here – What I haven’t said about my pregnancy. I’m going back to where I left off and doing bump progress shots, with more information about what we’ve learned along the way about our baby girl and her medical issue. All of these leading up to 33 weeks are written in past tense, just from what I remember was going on. I want a record for myself, for my little girl and to help anyone else who may find themselves in a similar situation.
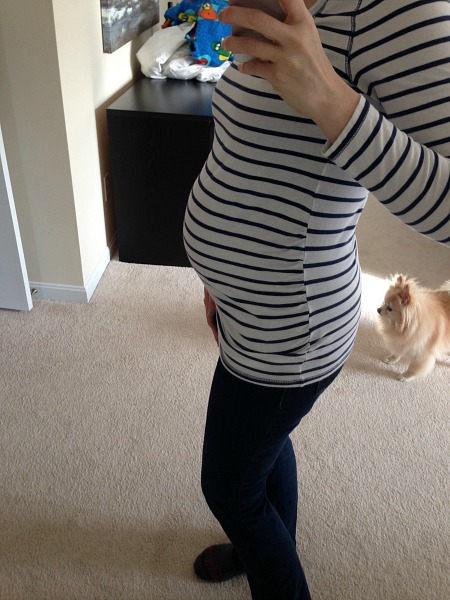
January 23rd – January 29th
How big is baby? She is now as big as a cantaloupe and is approximately 10.5-11.8″ long and 12.7-20.8 ounces. Still the same measurements, I think, so she’s just adding on fat and getting a little bigger. The Bump progress chart says this week her skin is becoming less opaque.
How I’m feeling? This was the week we went to Children’s for testing and multiple meetings, to get our surgical plan, post-operative care plan and a lot of other information. All of this happened in one day; we were at the hospital from about 8am until around 5pm or so. By the end of that day, we really did feel like we had as much information as we needed at the time to understand what was going to happen, but it was very overwhelming too.
The day started with an MRI. I’ve never had an MRI before so I wasn’t sure what to expect apart from things people have told me – loud, tight space where you have to be really still. Since this was happening at Children’s, the machine was decorated on the inside with stickers (balls of yarn, to be specific!) and there was also a tiny replica of the MRI machine in the room I was sent to to get ready.
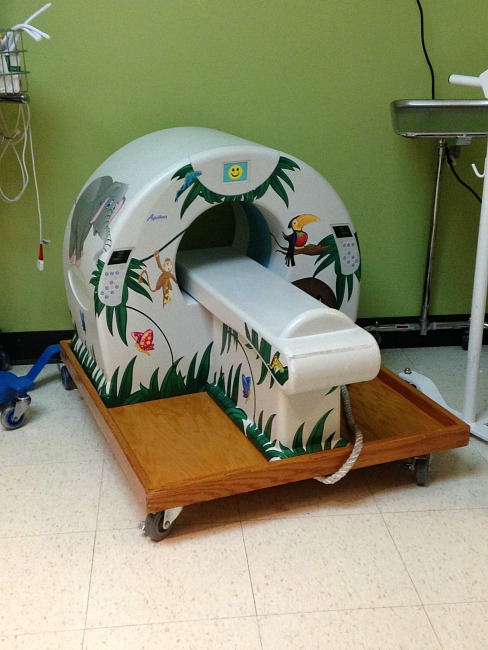
While I was in there, I kept thinking of the children who have to use the machine and how hard it must be to not be scared. Those machines are loud. It was unnerving, the sounds it made.
Following the MRI, we had the repeat echo which came back clear like the first one. After that, we grabbed some quick lunch and then headed up to wait for the string of meetings that had been scheduled for us. We met with a NICU nurse, a social worker and a genetic counselor. All of them were really informative and answered some of the questions we had. The big meeting, though, that we had been waiting for came after all of those – the surgical meeting.
In the surgical meeting, we met the surgeon (obviously), the neonatalogist, the high risk OB from another hospital (where I could switch my delivery to, but the OB said it wasn’t necessary since my hospital recently installed a level 3 NICU), and our nurse advocate. We went over the MRI images (which were the most incredible images I had ever seen. It was amazing to actually see my body from an aerial view, with the baby inside my belly and my organs all around her. With an ultrasound, you only see the baby but with this MRI, it was the whole picture. I wish I could get a copy of it, but there’s no way for me to view the images!) which showed exactly where the issue is inside the duodenum.
Doctors look at the duodenum in four segments, and the MRI revealed that our baby’s issue is isolated to the second section, which butts up against the pancreas. That could potentially complicate the surgery, but the surgeon emphasized it’s really just something to be aware of. We learned that the surgery could be laparoscopic or more invasive, depending on how serious the issue is. It could be either a total separation of the duodenum from the stomach, or the two could be connected but a blockage exists in the duodenum. If it’s the latter, it’s a less invasive surgery.
The surgeon estimated about a week for recovery from surgery, and at that point it would be safe to start working on occupational and/or speech therapy to help baby girl learn to take breastmilk by mouth. That means from the time I give birth until whenever we are home, I’ll be pumping full time. I’m really nervous about this because with Ezra, I did use a pump but I didn’t use it a lot and I remember not getting nearly as much milk with a pump as it seemed Ezra was getting.
Even more than that, I am nervous about not being able to breastfeed. What if she never learns to latch? I know bottle feeding is not the end of the world, but breastfeeding is one of those things that is really important to me. But, for now, I guess it does no good to stress about it.
Any cravings or weird dreams? I think it was around this time that I started craving salads even more. I was already craving them here and there, but I distinctly remember wanting them so much that they would even make appearances in my dreams (so weird). Just any kind of salad, really, covered in some delicious dressing.
Any other details? No, because this week had so much information that we were pretty brain dead by the end. It was all good information, though, and we walked away from that day at Children’s feeling really good about our girl’s outcome, about the team caring for her and about the future.
I had gotten a few details from the OB present at the meeting about what to expect for pregnancy and delivery. So far, everything he’s said has happened. Polyhydramnios (aka, excess amniotic fluid) is the most stressful side effect, if you want to call it that, that effects pregnancy in this case and I’ve been dealing with it at a large level for about a month now. The OB also said that most babies with DA don’t make it full term, and on average tend to arrive around 36 weeks (which now I understand is because of the excess fluid – it irritates the uterus and causes contractions). He mentioned that nonstress tests and amniotic fluid indexes would be regular occurrences (twice a week!) as well as growth ultrasounds every 3-4 weeks to make sure the baby continues to stay on track.
The neonatalogist went over the post-delivery/pre-surgery/post-surgery side of things. We were really happy to learn that there wouldn’t be too much of a rush after delivery to get her transported to Children’s – we will likely have 2-3 hours with her before she has to go to the NICU. Once she is in the NICU, she’ll be fed via IV and will be intubated to decrease the chance of her taking in air to her belly (because she has no way of getting that air back out). He talked about kangaroo care, pumping, etc.
So.much.information but all very good. Nights when I can’t sleep, I go back over that meeting and talk myself through everything. Surprisingly, it helps, plus it keeps the details fresh. I really can’t say enough good things about Children’s Hospital and the people we’ve worked with so far. I feel incredibly lucky that they will be taking care of our daughter.



Leave a Reply